Medicare Criteria For Home Health: What Does “HOMEBOUND” Mean?
Medicare requires that a patient be “homebound” and have a “skilled need” to qualify under Medicare for home health nursing and therapy services. Medicare considers you homebound if:
- You need the help of another person or medical equipment such as crutches, a walker, or a wheelchair to leave your home.
- Your doctor believes that your health or illness could get worse if you leave your home.
Here are some tips to help you decide if your patient meets Medicare requirements…
Homebound Definition
“Homebound” does NOT mean that a patient has to be “bed-bound” to qualify. The patient is considered “homebound” under Medicare if the patient cannot leave home without “considerable and taxing effort.”
Most patients have an injury or illness that makes it difficult to leave home; for example, if the patient:
- Requires the aid of supportive devices (wheelchair or walker)
- Requires the use of special transportation
- Needs the assistance of another person
- Has a condition where leaving the home is medically contraindicated
- Symptoms of the disease process (such as pain, shortness of breath, or confusion) worsen when leaving the home
Qualified Trips
The patient can leave home for medical treatment (such as chemotherapy or dialysis) or for receiving therapeutic and psychosocial treatment (such as through a certified adult day care program).
The patient cannot be disqualified from services if they leave home for a non-medical absence as long as the absence is “infrequent and short in duration.” Some examples include attending a religious service, a trip to the barber, a special family event, or a walk around the block.
Signature Health Services has delivered exceptional skilled nursing and licensed therapy services to more than 25,000 homebound patients, partnering with 4,000 physicians, for over 25 years. Signature has received Medicare’s coveted 4.5-star rating for the best in quality of care, and a 100% Compliance audit score from the Texas Health and Human Services Commission for meeting all State and federal Medicare standards.

We Are Here to Help
ALWAYS ON CALL
| Monday – Sunday | 24 / 7 |
1 (800) 277-8291 (option 1)
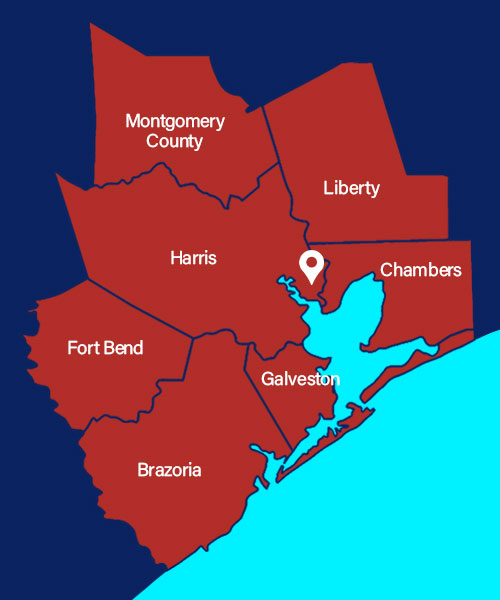
COUNTIES SERVED
OUR VALUES
TESTIMONIALS

I love all of my home health people.

All Signature staff as well as therapy were very helpful.

Their services have always been great.

I really love my physical therapist. Gary has helped me so much.

This has been one of the best agencies. Very caring nurses.

I’ve had a really good physical therapist and really nice nurses.

I have had excellent care & would recommended them to anyone.

Gary Dixon is the very best physical therapist in Baytown and Houston Area.