For people and families impacted by cervical disease, understanding cervical health awareness goes beyond statistics. It is about the difference that education, prevention, and supportive care can make in quality of life and long-term health outcomes. Cervical conditions are among the most preventable cancers, and with the proper tools and care, many cases can be addressed before they advance to invasive disease.
At Signature, we know that involvement of trained healthcare professionals, such as nurses and therapists, can support people through preventive care, screening reminders, recovery coordination, and compassionate education. These efforts strengthen cervical cancer prevention programs and help families make informed choices about their health.
What Cervical Cancer Is and Why It Matters
Cervical cancer develops in the cells of the cervix, the narrow lower portion of the uterus that connects to the vagina. Nearly all cervical cancers are linked to persistent infection with high-risk types of human papillomavirus (HPV), a common virus transmitted through intimate contact. Most HPV infections resolve on their own. However, when high-risk strains remain over time, they can change cervical cells and lead to cancer if not detected and treated.
In the United States, approximately 13,360 new cases of cervical cancer were diagnosed in 2025, and about 4,320 women died from the disease, according to national cancer data. Cervical cancer continues to be a significant health issue despite long-standing screening and prevention efforts.
Achieving cervical screening awareness is an essential step in reducing these numbers.
Why Screening Is Fundamental to Prevention
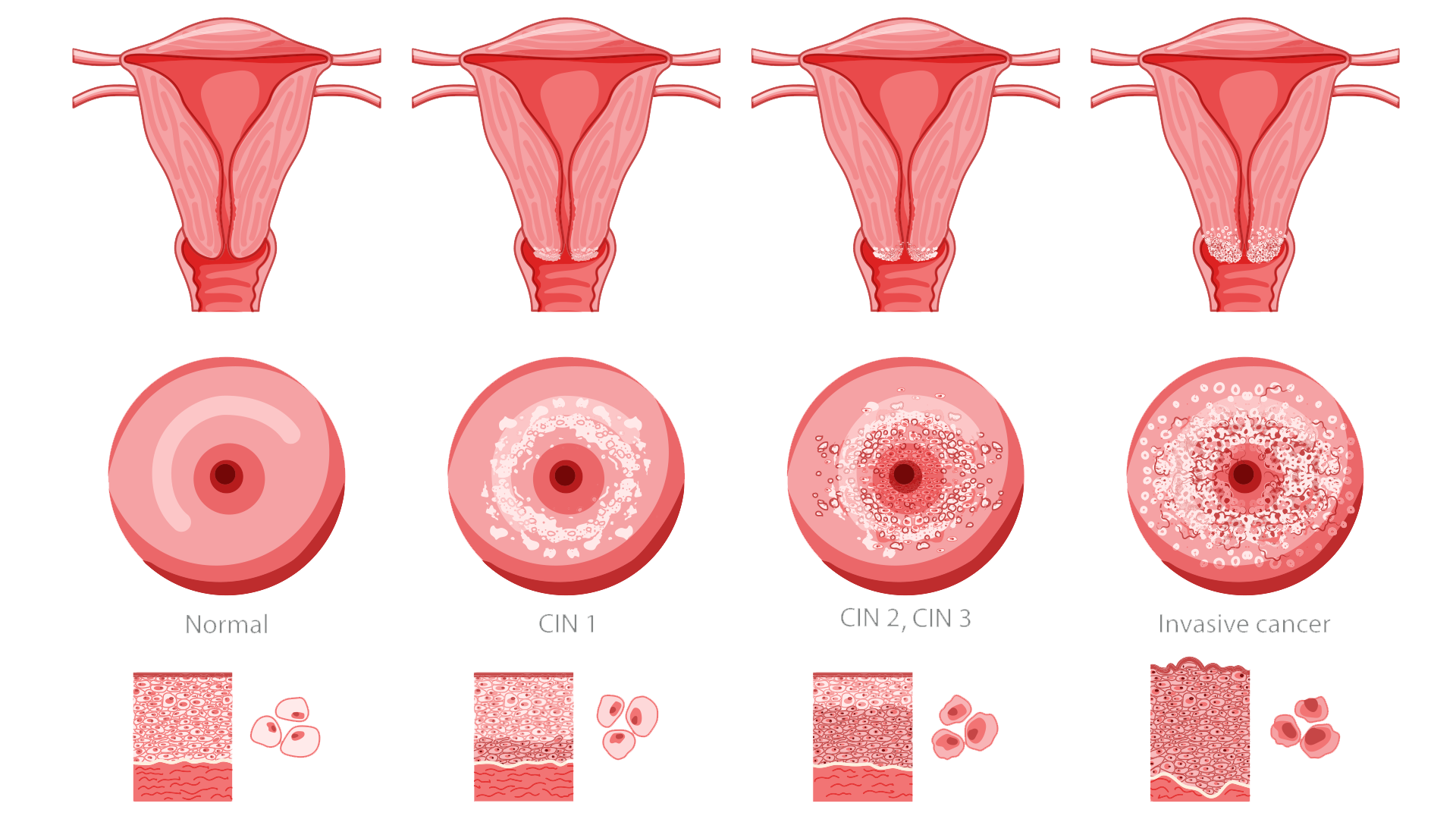
One of the greatest advances in controlling cervical cancer has been the development and widespread use of regular screening tests. These tests are designed to detect precancerous changes before they develop into invasive cancer. Early identification of these in-between changes allows for treatment that prevents progression.
Two primary forms of screening are widely used:
Increasingly, new options such as self-collected HPV testing kits, including at-home sampling tools, are becoming available and may help reduce barriers to participation in routine screening.
Role of HPV Vaccination in Cervical Cancer Prevention
Vaccination against HPV is a major component of cervical cancer prevention programs. HPV vaccines protect against the high-risk virus types most likely to cause cervical cancer and other related cancers.
Vaccines are most effective when given before exposure to HPV. Initially recommended primarily for adolescents, vaccination guidelines have expanded to cover a wider age range. Although public health recommendations continue to evolve, the data show that vaccination and screening together have dramatically reduced the prevalence of precancerous lesions and the risk of cancer in vaccinated populations.
As vaccination rates increase and screening becomes more accessible, the broader goal of drastically lowering cervical cancer incidence moves closer to reality (more information).
Why January Cervical Health Awareness Month Matters
Every January, Cervical Health Awareness Month takes place, and organizations across the United States and globally emphasize the importance of education, screening, and prevention. This period highlights the impact of these combined strategies and encourages communities to engage in practices that protect long-term well-being.
For families and caregivers, this awareness can prompt conversations with primary care providers about appropriate screening schedules, risk factors, and preventive steps.
Early Detection Saves Lives
The dramatic decline in cervical cancer incidence and mortality over recent decades is largely due to early detection through screening and HPV vaccination. When cervical cancer is identified at a localized stage, the five-year relative survival rate in the United States exceeds 90 percent.
Regular screening does more than identify existing cancers. It can uncover changes in cervical cells that indicate future risk. Addressing these changes early can prevent cancer altogether. This is why cervical screening awareness is such a critical public health message.
Home Nurses and Therapists: Enhancing Care at Every Step
For patients living with precancerous cervical changes, a history of HPV, or a cancer diagnosis, having a supportive care team makes a real difference. Home nurses and therapists contribute in multiple ways:
This personalized approach improves adherence to recommended care and fosters confidence and comfort for patients and families.
Toward a Future With Less Cervical Cancer
Thanks to ongoing advances in screening technology, improved understanding of HPV biology, and stronger vaccination efforts, the future holds promise for further reductions in cervical cancer burden. Increasing access to care and continuing public education remain central to achieving these goals.
By integrating cervical health awareness into community health practices year-round and reinforcing key messages during January, we collectively support healthier outcomes for individuals and communities.
At Signature Health Services, we are committed to supporting our patients and their loved ones through every stage of cervical health care. Whether through education, care coordination, or emotional support, our home nursing and therapy teams stand with you.
Call Signature 24/7 at 800-277-8291 for excellence in skilled and compassionate home health care.

Your Complete Home Health Care Solution!
ALWAYS ON CALL
| Monday – Sunday | 24 / 7 |
1 (800) 277-8291 (option 1)
COUNTIES SERVED
OUR VALUES
TESTIMONIALS

I love all of my home health people.

All Signature staff as well as therapy were very helpful.

Their services have always been great.

I really love my physical therapist. Gary has helped me so much.

This has been one of the best agencies. Very caring nurses.

I’ve had a really good physical therapist and really nice nurses.

I have had excellent care & would recommended them to anyone.

Gary Dixon is the very best physical therapist in Baytown and Houston Area.